Denial Management Service
Revex Square’s Denial Management service identifies claim issues, corrects coding errors, appeals denials promptly, and prevents future rejections streamlining your revenue cycle and securing payments with less effort.
Advanced Denial Management Solutions
At Revex Square , we understand the vital role denial management plays in the revenue cycle. It acts as a safety net for medical providers and billing companies, correcting errors in early revenue steps. That’s why our team specializes in managing denied claims and prioritizing effective Accounts Receivable (A/R) Management.
By focusing on low account receivables through timely appeals and reimbursements, healthcare providers can maintain streamlined workflows and faster collections. Our denial management services directly address medical claim rejections, ensuring efficiency in your revenue cycle. With Revex Square , your practice benefits from tailored, comprehensive A/R management solutions.

Other Service
Comprehensive healthcare Medical solutions for your specialities
Take the First Step to Multiply Your Revenue
Let’s turn your business potential into real profit
Why Choose Revex Square?
Pioneering Affordable,
All-Inclusive RCM Solutions
- Over 99% Claims Approved
- Less than 1% Rejection Rate
- Seamless HIPAA Compliance
- Rates Begin at Just 2.95%
- Rigorous Practice Billing Audits
- Unmatched Error Reduction
- Enhanced Cash Flow
Claim Accuracy
10
+
States Served
10
+
Happy Clients
10
+
Specialties Expert
10
+
Denial Management Process
Revex Square reduces the burden and cost of administrative work for medical practices. Because billing is complex and time-consuming, staff can become overwhelmed. Outsourcing to our expert team streamlines operations and improves financial outcomes, allowing providers to stay focused on patient care.
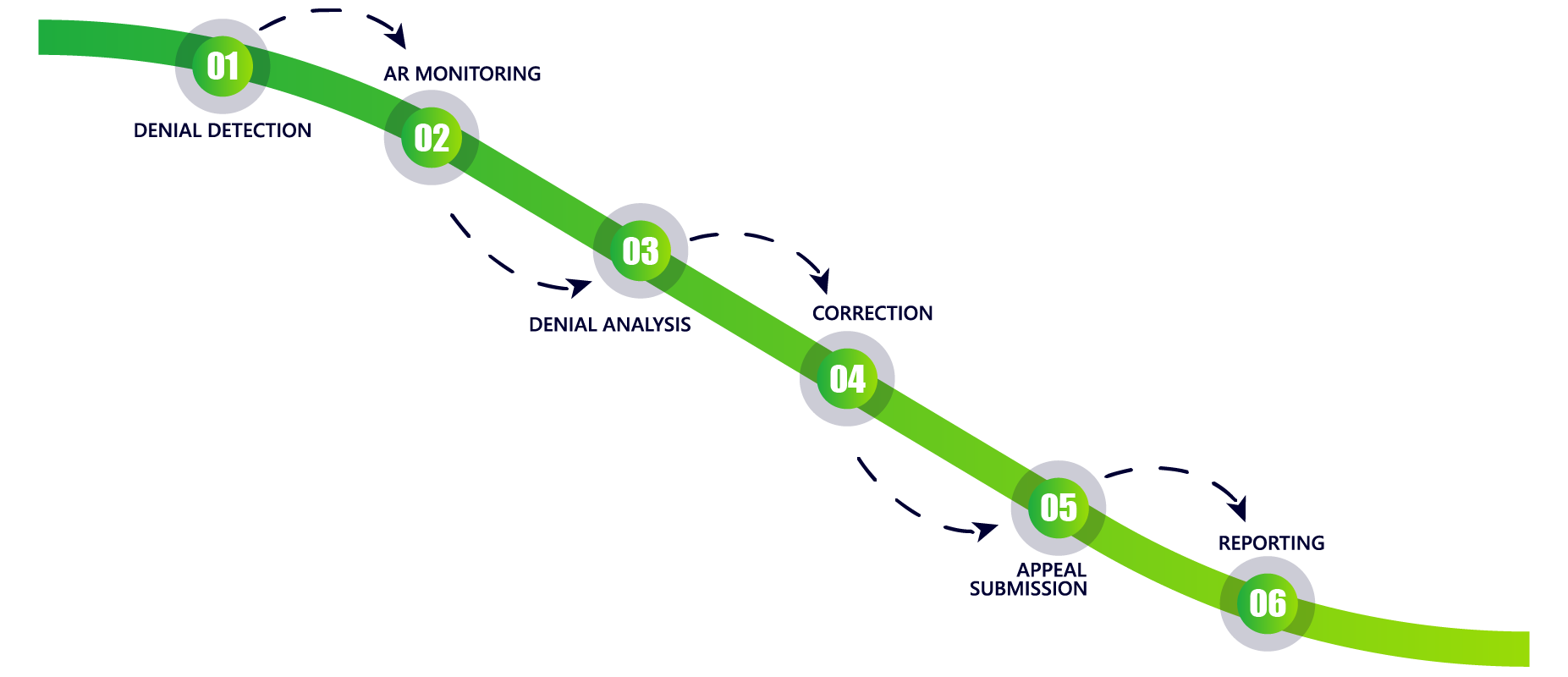
Benefits of Denial Management Services
Streamlined Enrollment
We manage each step of credentialing, ensuring fast, accurate enrollment from start to finish.
Compliance Assurance
Our rigorous process guarantees full regulatory compliance and minimizes audit-related risks.
Time & Cost Efficiency
Save valuable time and operational costs by outsourcing credentialing to our trusted experts.
Faster Payment Cycles
EFT and ERA integration simplifies payment posting and accelerates overall revenue flow.
Dedicated Expert Support
Our credentialing specialists offer hands-on support to guide you through every stage.
Error-Free Applications
We eliminate credentialing errors, ensuring all applications are accurate and accepted quickly.
Our Comprehensive Denial Management Service in USA
Denial Analysis & Identification – Thorough review of denied claims to identify root causes, including coding errors, eligibility issues, or missing information.
Claim Correction & Resubmission – Accurate correction and prompt resubmission of denied claims to ensure faster reimbursement and minimal revenue loss.
Denial Prevention Strategies – Implementation of proactive measures, including workflow improvements and staff guidance, to reduce future claim denials.
Compliance & HIPAA Security – Fully HIPAA-compliant denial management processes to ensure secure handling of patient and insurance data.
Custom Denial Management Solutions – Tailored services designed for small practices, clinics, hospitals, and large healthcare organizations across the USA.

0
%
Satisfied Clients
Starting from 2.75%

Denial management Services Near Me
Searching for a “Denial management services near me”? Revex Square proudly serves healthcare providers across the USA with dedicated support teams, ensuring a local feel with national expertise. Our team understands the unique billing challenges faced by American healthcare providers and offers solutions tailored to your region and specialty.


President
Revex Square’s team is impressively responsive—always addressing within hours. They fight hard with insurance companies to ensure we receive full reimbursements. They also quickly mastered our chiropractic software and integrated seamlessly into our workflow. Their service is reliable, efficient, and fairly priced—I couldn't be more satisfied.

Pediatrics
Partnering with Revex Square has been a game-changer for our practice. In just six months, they cleared our AR backlog and dramatically improved our billing operations. Their professionalism, attention to detail, and responsiveness have exceeded our expectations. Our practice is now running more efficiently than ever—thank you, Revex Square!